Anahita Kodali, Medical Sciences, News, Spring 2020
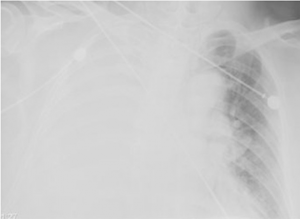
Figure 1: Another test for microbial invasion is looking for pleural effusion, or a buildup of fluid on the lungs. This image shows pleural effusion of the right lung.
Image Source: Wikimedia Commons
Sepsis is the body’s extreme reaction to an already existing infection. Normally, when someone has an infection, their body’s immune system is able to naturally care for it by sending chemicals into the bloodstream to fight it off. However, sometimes, the chemicals released cause widespread inflammation instead, resulting in sepsis. If left untreated, sepsis progresses to septic shock, causing a potentially fatal drop in blood pressure.1 While sepsis can be life threatening to anyone, it is most dangerous for adults over 65, children younger than a year, people who are immunocompromised, and people with preexisting chronic medical conditions.2
Sepsis is a particularly challenging issue for physicians and researchers to deal with because treatment efficacy is dependent on early diagnosis. However, it is very difficult to catch sepsis early. Diagnosis for sepsis is usually dependent on three things: onset of clinical symptoms when the patient responds to sepsis (including fever, chills, and changes in white blood cell counts), signs of infection (including smelly urine, respiratory symptoms, and signs of meningitis), and microbial invasion of a usually sterile environment (to test this, physicians can give a peritoneal tap to patients, which drains excess fluid from the abdomen, to see if this invasion has occurred). The problem is that not all these indications are always present. In addition, critically ill patients ( who are most at risk for sepsis) often have several of these indications prior to actually developing sepsis, and some of the treatments they receive for their other conditions cause tests for sepsis to run fall positives or negatives.3Thus, physicians usually cannot diagnose sepsis until the first symptoms start to appear.
To address these issues, researchers from TU Graz’s Institute of Computational Biotechnology have developed a diagnostic tool that can catch sepsis as much as three days before the first symptoms of sepsis set in. The team used sequencing tools and data to study plasma samples from healthy people and those diagnosed with sepsis caused by bacterial infection or fungal infection. The researchers were able to identify 24 biomarkers that characterized early sepsis and could distinguish a person with normal clinical symptoms from someone with sepsis, solving many of the hurdles that prevent physicians from quickly diagnosing sepsis.4 In an interview with ScienceDaily, the researchers stated their test had an accuracy rate of 90%.5
Undoubtedly, this data and new test has incredible potential for physicians and researchers studying sepsis alike. Hopefully after its widespread implementation, hopefully there will be a dramatic reduction in the number of deaths related to sepsis.
Bibliography
[1] Sepsis. (2018, November 16). Mayo Clinic. Retrieved from https://www.mayoclinic.org/diseases-conditions/sepsis/symptoms-causes/syc-20351214
[2] What is sepsis? (2019, August 27). CDC. Retrieved from https://www.cdc.gov/sepsis/what-is-sepsis.html
[3] Vincent J-L (2016) The Clinical Challenge of Sepsis Identification and Monitoring. PLoS Med 13(5): e1002022. https://doi.org/10.1371/journal.pmed.1002022
[4] Elisabeth Ullrich, Petra Heidinger, Jung Soh, Laura Villanova, Stefan Grabuschnig, Thorsten Bachler, Elisabeth Hirschböck, Sara Sánchez-Heredero, Barry Ford, Maria Sensen, Ingund Rosales Rodriguez, Daniel Schwendenwein, Peter Neumeister, Christoph J. Zurl, Robert Krause, Johannes Lorenz Khol, Christoph W. Sensen. Evaluation of host-based molecular markers for the early detection of human sepsis. Journal of Biotechnology, 2020; 310: 80 DOI: 10.1016/j.jbiotec.2020.01.013
[5] Graz University of Technology. (2020, April 21). Milestone for the early detection of sepsis. ScienceDaily. Retrieved April 22, 2020 from www.sciencedaily.com/releases/2020/04/200421112512.htm